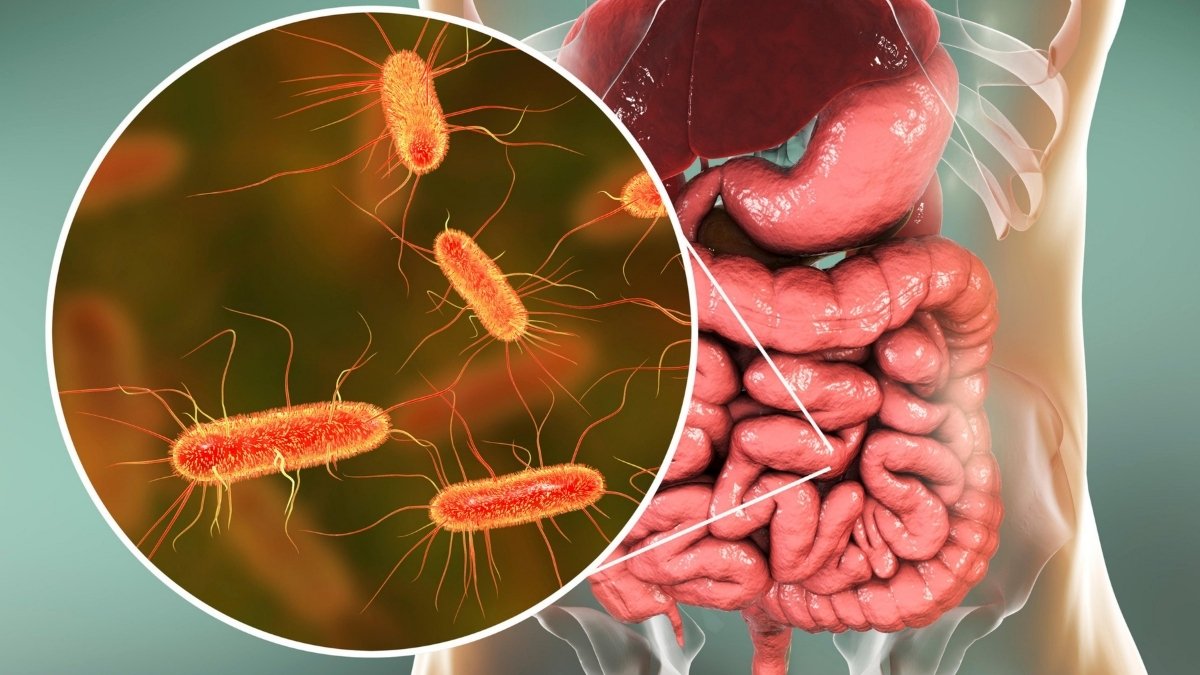
Feeling foggy-headed lately? Can’t seem to think clearly no matter how much coffee you drink? Your gut bacteria might be the culprit.
Most people don’t connect their mental clarity issues with what’s happening in their digestive system. But science now shows a powerful link between gut health and brain function.
The trillions of microbes living in your intestines constantly communicate with your brain, influencing everything from mood to memory.
Left unchecked, an unhealthy gut microbiome can sabotage your mental sharpness without you even realizing it. Here are 11 warning signs to watch for – and what you can do about them.
1. Chronic Brain Fog
Your gut microbes play a crucial role in brain function. When bacterial balance goes awry, neurotransmitter production suffers.
These chemical messengers like serotonin and dopamine can’t work properly when gut health falters. Harmful bacteria release toxins such as lipopolysaccharides that trigger body-wide inflammation.
This inflammation doesn’t stay put in your gut – it travels through your system and disrupts neural communication pathways. The result? That frustrating mental cloudiness that makes thinking feel impossible.
The connection works both ways. Good bacteria produce compounds that strengthen your blood-brain barrier, while an unhealthy gut weakens this protection.
Many people notice their thinking sharpens when they improve their gut health through diet changes. Small shifts in what you eat can lead to big improvements in mental clarity.
2. Persistent Fatigue

Feeling constantly tired might be traced back to your gut bacteria. An imbalanced microbiome produces fewer short-chain fatty acids like butyrate, which your brain cells need for energy production.
Think of these compounds as premium fuel for your mental engine. Your gut bacteria influence how your body handles inflammation.
When bad bacteria outnumber the good ones, inflammatory molecules increase throughout your body. This creates what scientists call “inflammatory fatigue” – a dragging exhaustion that doesn’t improve with rest alone.
Your brain requires massive energy to function well, making it particularly vulnerable. The tiredness often comes in patterns. You might feel somewhat normal in the morning but crash by afternoon. Or perhaps you wake up exhausted despite sleeping enough hours.
Many people report their energy levels stabilizing when they address gut health issues. Simple changes to diet and lifestyle can help restore bacterial balance and reduce fatigue.
3. Mood Swings or Irritability

Your gut bacteria influence your emotions more than you might think. About 90% of serotonin – your “feel good” neurotransmitter – gets produced with help from gut microbes.
When certain beneficial bacteria decrease, your mood regulation system becomes unstable. Low levels of helpful bacteria like Lactobacillus and Bifidobacterium link directly to erratic emotional changes.
These bacteria help create the building blocks your body needs to make mood-stabilizing chemicals. Without them, your emotional responses can swing wildly from calm to irritated with little provocation.
The gut-mood connection explains why you might feel irritable after eating certain foods. Some people notice dramatic mood improvements after changing their diet or taking probiotics.
Your emotions aren’t just “all in your head” – they’re partially created in your digestive system. This biological reality means gut health strategies can sometimes help stabilize mood more effectively than willpower alone.
4. Anxiety or Depression

The link between gut bacteria and mental health grows stronger with each new study. Your microbiome affects how your body processes stress hormones and neurotransmitters that regulate mood.
When certain bacterial species decline, your brain’s ability to maintain emotional balance suffers. Some bacteria produce compounds that act as natural antidepressants.
Your gut contains an entire ecosystem that helps determine whether you feel mentally well or unwell. People with depression often show distinct patterns in their gut bacteria populations compared to those without mood disorders.
These differences appear consistently across various studies. Food choices directly shape your internal bacterial community.
Eating processed foods, sugar, and artificial ingredients tends to promote bacteria that worsen mood. Meanwhile, vegetables, fermented foods, and fiber support bacteria that produce mood-boosting substances.
This connection partly explains why diet changes sometimes help with anxiety and depression symptoms when other approaches fall short.
5. Poor Sleep Quality

Your gut bacteria help control your sleep-wake cycle in surprising ways. Beneficial microbes produce sleep-supporting substances like GABA and melatonin – the same compounds many sleep supplements contain.
When your microbiome falls out of balance, this natural production process breaks down. Night after night of tossing and turning might signal a gut issue.
Some bacteria affect circadian rhythms directly, telling your body when to feel alert and when to feel sleepy. Others influence how your body handles stress, which impacts sleep quality.
Many insomnia sufferers have unusual bacterial patterns in their digestive systems. Sleep problems and gut issues often form a vicious cycle. Poor sleep worsens gut health, and gut problems disrupt sleep.
Breaking this cycle typically requires addressing both sides of the equation. Many people find their sleep improves when they make gut-friendly changes like limiting sugar, eating earlier in the evening, and increasing fiber intake.
6. Sugar Cravings

Those intense urges for sweets might come from the microbes in your gut. Certain harmful bacteria and yeasts like Candida thrive on sugar and can manipulate your hunger signals.
They essentially hijack your nervous system, creating powerful cravings that benefit them rather than you. This creates a troublesome cycle – eating sugar feeds these problematic microbes, allowing them to multiply and send even stronger craving signals.
Many people describe these urges as feeling different from normal hunger. They often come with specific demands for particular sweet foods, sometimes at odd times.
The good news? This cycle can be broken. As you change your diet to include more fiber and fewer refined sugars, your microbial population shifts.
Beneficial bacteria increase while sugar-loving ones decrease. People commonly report that their sugar cravings diminish significantly after a few weeks of gut-friendly eating.
Your food preferences aren’t just habits – they’re partly determined by which microbes dominate your digestive system.
7. Digestive Issues (Bloating, IBS)
Ongoing digestive problems often signal gut bacteria imbalances that affect your brain. When your intestinal barrier weakens, bacterial toxins like LPS can leak into your bloodstream. This triggers inflammation not just in your gut, but throughout your body and brain.
A 2023 study found a direct connection between IBS symptoms and altered gut microbiota. Researchers discovered that people with IBS often have high levels of certain bacteria like Streptococcus and experience anxiety alongside their digestive symptoms.
This wasn’t coincidental—the same bacterial patterns linked to both conditions. Bloating, gas, constipation, and diarrhea might seem like purely digestive concerns, but they often coincide with brain fog and mood changes.
Your gut and brain communicate constantly through the vagus nerve and other pathways. Addressing these digestive symptoms frequently improves mental clarity.
Many find that eliminating certain foods, adding probiotics, or using specific herbs can help break this cycle and clear thinking returns as gut symptoms improve.
8. Frequent Headaches or Migraines

Headaches that come regularly might originate in your gut. Gut inflammation caused by bacterial imbalances can activate the trigeminal nerve, which plays a key role in migraine development.
This neural pathway creates a direct communication line between your digestive system and your head pain. Some bacterial species trigger inflammation and release histamine, a known headache culprit.
People with certain bacterial patterns, particularly those with high levels of Prevotella, experience more frequent migraines.
Your gut bacteria also influence how you process foods that might trigger headaches, like aged cheese, wine, and chocolate.
Many headache sufferers find relief when they work on their gut health. Eliminating inflammatory foods, addressing bacterial overgrowth, and supporting healthy bacteria can reduce headache frequency and intensity.
Some doctors now recommend stool tests for patients with chronic headaches to identify potential bacterial contributors.
The connection explains why many migraine medications cause digestive side effects—they’re influencing the same neural pathways that connect these two systems.
9. Memory Problems

Forgetting where you put your keys or blanking on names might trace back to your gut. Your brain relies on compounds called short-chain fatty acids, such as butyrate, which specific types of bacteria create.
These substances play a key role in helping the hippocampus form memories properly. Without enough of these helpful microbes, your brain struggles to build and maintain neural connections needed for remembering.
Low microbial diversity, common in Western diets high in sugar and processed foods, reduces the production of these memory-supporting compounds.
Your gut bacteria also influence inflammation levels throughout your body. Chronic inflammation damages brain tissue over time, particularly in areas responsible for memory.
Some people notice their memory sharpens when they improve their gut health. Adding fermented foods, fiber-rich vegetables, and reducing sugar intake can promote bacterial balance.
Omega-3 fatty acids found in fish and certain seeds support both gut health and memory function. This explains why traditional diets high in fermented foods and plant fiber are associated with better cognitive health in old age.
Your memory isn’t just about what’s happening in your brain—it’s strongly influenced by the bacterial community in your gut.
10. Difficulty Concentrating

Struggling to stay focused on tasks might be connected to your gut bacteria. Your microbiome directly influences dopamine production and regulation—a neurotransmitter essential for concentration, motivation, and mental clarity. Without proper bacterial balance, these attention systems falter.
A 2017 study examining probiotics containing Bifidobacterium found they improved focus and attention in mice by modulating dopamine receptors.
The researchers noted that the effect was comparable to certain medications used for attention disorders. This research suggests bacterial composition could be a previously overlooked factor in concentration problems.
The gut-brain connection works both ways when it comes to focus. Stress makes it harder to concentrate and simultaneously disrupts the gut-bacterial balance.
This creates a cycle where poor concentration leads to stress, which worsens gut health, further impairing concentration.
Breaking this cycle often requires addressing both mental and digestive aspects. Many people report clearer thinking after several weeks of gut-supportive diet changes, particularly reducing sugar and artificial ingredients while increasing fiber and fermented foods.
11. Unexplained Weight Changes

Mysterious shifts in your weight might stem from gut bacterial imbalances affecting both your metabolism and brain function.
Certain bacterial populations influence how efficiently you extract calories from food and how your body stores fat. They also affect hunger hormones that control your appetite.
Microbiomes dominated by Firmicutes bacteria are linked to both weight gain and cognitive symptoms like brain fog.
These bacteria extract more calories from food than other types, potentially leading to weight gain even without eating more. At the same time, they can contribute to inflammation that clouds thinking.
Changes in weight without obvious cause often frustrate people who don’t understand the gut connection. Your eating habits aren’t solely determined by willpower—they’re influenced by chemical signals from gut bacteria.
Some bacteria increase cravings for foods that feed them while others promote feeling satisfied with less food.
Addressing bacterial imbalances through diet, prebiotics, probiotics, and lifestyle changes often helps stabilize weight while simultaneously improving mental clarity. The two improvements frequently happen together because they share the same root cause.