It’s 3 AM. You’re wide awake, and your heart is doing… something. A flutter. A skip. A forceful thump that echoes in your ears. If you’re a woman over 45, you’ve likely been told it’s just anxiety or a normal part of the menopausal transition.
But cardiologists are now warning about a specific “bedroom habit” that is a direct line to these terrifying nighttime heart palpitations.
What is this habit? It’s the habit of ignoring the subtle symptoms of a serious condition: Obstructive Sleep Apnea (OSA).
You might think, “I don’t snore like a freight train, so that’s not me.” But here’s the critical link: sleep apnea presents differently in women over 45.
Its symptoms are often mistaken for menopause, and this habit of overlooking it is putting millions of women’s hearts at risk.
This article will break down the proof, show you the subtle signs to look for, and give you the actionable steps to take back control of your heart health, starting tonight.
Why Do Heart Palpitations Spike for Women Over 45?

Why now? Why does it seem like your body’s check-engine light suddenly clicks on after 45? It often comes down to a perfect storm of hormones and misdiagnosis.
First, the hormone connection. The female hormones estrogen and progesterone play a protective role in your breathing.
They help maintain muscle tone in your upper airway. As these hormones decline during perimenopause and menopause, the tissues in your throat are more likely to relax and collapse while you sleep.
This hormonal shift is why studies show that postmenopausal women are two to three times more likely to develop sleep apnea than premenopausal women.
The problem is, the symptoms of this new-onset sleep apnea look exactly like the classic symptoms of menopause.
Doctors and women alike see night sweats, insomnia, anxiety, and fatigue and blame them on “the change.” The heart palpitations are then dismissed as a side effect of this new anxiety.
But here’s what’s really happening: The “anxiety” isn’t the primary cause; it’s a symptom. It’s your body’s panic response from repeatedly not being able to breathe.
While hormonal flutters are certainly real, a persistent, thumping, or skipping heartbeat that worsens at night points to something more.
The “Habit” Explained: Ignoring Atypical Sleep Apnea

When you think of sleep apnea, you probably picture a man with loud, gasping snores who falls asleep at his desk. This stereotype is the single biggest reason sleep apnea in women is overlooked.
The “habit” cardiologists warn against is seeing the real symptoms in yourself and dismissing them as just ‘part of being a woman over 45.’
According to the National Heart, Lung, and Blood Institute (NHLBI), women’s symptoms are often more subtle and less about snoring. Instead of loud, disruptive snoring, women are more likely to report:
- Insomnia: Specifically, the inability to stay asleep. You wake up repeatedly for “no reason.”
- Waking up with a headache: A dull, throbbing headache first thing in the morning.
- Chronic daytime fatigue: A deep, profound exhaustion that coffee doesn’t fix. It’s not just “tired”; it’s “depleted.”
- New or worsening anxiety or depression: Suddenly feeling overwhelmed, moody, or panicked, especially at night.
- Waking up gasping: A sudden jolt awake, feeling short of breath, often with a racing heart (this is the palpitation itself).
- Night sweats: Waking up drenched in sweat that isn’t related to a typical hot flash.
You look at this list and think, “That’s just my life. That’s just menopause.” This habit of ignoring these signs means the underlying cause—your body stopping breathing dozens or even hundreds of times a night—goes completely untreated.
The Medical Proof: How Sleep Apnea Directly Causes Palpitations
This isn’t a vague “link.” There is a direct, physical chain of events that connects sleep apnea to heart palpitations. Here’s what I mean.
It happens like this, night after night:
- The Airway Collapses: You fall asleep, and the muscles in your throat relax and collapse, blocking your airway.
- Breathing Stops: For 10, 20, or even 30+ seconds, you are not breathing. This is an “apnea” event.
- Oxygen Plummets: Your blood oxygen levels drop dramatically. This is a condition called hypoxia.
- The Brain Panics: Your brain, sensing a life-threatening emergency, hits the alarm button. It floods your body with stress hormones like adrenaline and cortisol to shock you awake just enough to take a breath.
- The Heart Pays the Price: This nightly flood of stress hormones, combined with the low oxygen and intense changes in chest pressure, directly irritates your heart’s electrical system.
You could say it’s like your heart is being put through a nightly stress test it never signed up for. The result is the flutter, skip, or pound you feel.
These are often premature ventricular contractions (PVCs) or, more dangerously, atrial fibrillation (AFib).
That’s the real danger. Research consistently shows that people with untreated sleep apnea are 2 to 4 times more likely to develop AFib, a major arrhythmia that can lead to stroke.
And with an estimated 80% of moderate to severe sleep apnea cases still undiagnosed, this is a silent epidemic.
Your 2025 Action Plan: How to Stop the Habit and Protect Your Heart

So, what can you do about it? Right now. Tonight. You can break the habit of passivity and take control. Here is your 2025 action plan.
Step 1: Self-Assessment (The First 5 Minutes) Stop wondering and start gathering data. Ask your partner, “Have you ever heard me gasp for air or stop breathing in my sleep?” If you sleep alone, use a sleep-tracking app on your phone. Many can record audio and will flag periods of loud snoring or the tell-tale silence followed by a gasp.
Step 2: Talk to Your Doctor (The Right Way) Do not go to your doctor and just say, “I’m tired and anxious.” You will likely be given a prescription for anxiety or sleeping pills, which can make sleep apnea worse.
Instead, advocate for yourself. Use this exact phrase: “I am a woman over 45 experiencing heart palpitations, chronic fatigue, and insomnia. I am concerned about atypical sleep apnea and I would like a referral for a sleep study.”
This specific language shows you’ve done your research and moves you past the “menopause” dismissal. Many sleep studies can now be done conveniently at home.
Step 3: Lifestyle Habits to Start Tonight (Actionable) While you wait for a diagnosis, these steps can provide immediate relief:
- Change Your Position: Most apnea is worse when sleeping on your back. Use a body pillow (or the old “tennis ball in the back of your pajamas” trick) to force yourself to sleep on your side.
- Avoid Alcohol Before Bed: Alcohol is a muscle relaxant. That glass of wine to “help you sleep” is actually making your airway more likely to collapse. Stop all alcohol at least 3 hours before bed.
- Manage Weight: This is crucial. Even a 10% reduction in body weight can dramatically reduce the severity of sleep apnea by decreasing fatty tissue around the airway.
Step 4: Understand Modern Treatment (It’s Not Just a Mask) If you are diagnosed, the news is good. This is 100% treatable. In 2025, your options are better than ever:
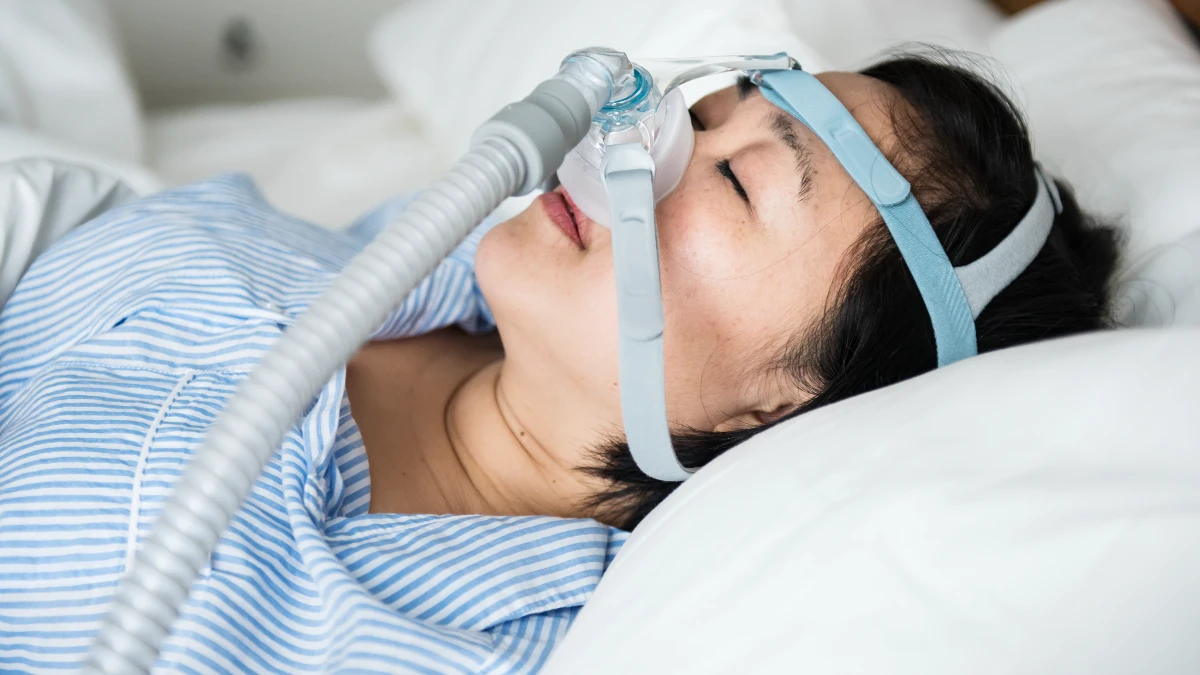
- CPAP: Still the gold standard, but today’s machines are silent, small, and use comfortable, minimalist masks (like nasal pillows).
- Oral Appliances: For mild-to-moderate OSA, a sleep dentist can create a custom mouthguard (a mandibular advancement device) that gently moves your lower jaw forward, keeping your airway open. No mask, no machine.
- Hypoglossal Nerve Stimulation: This is a newer, implantable device (like a pacemaker) that stimulates your tongue muscle to move forward when you breathe, keeping the airway clear.
The “I’m Not Anxious” Script: How to Advocate for a Sleep Study

This is often the most frustrating part of the journey. You describe a terrifying, physical sensation—a heart that skips, thumps, and races—and you are told it’s “just anxiety.”
You may be offered an antidepressant or a sleeping pill, which can actually make sleep apnea worse.
It’s invalidating. To get the right test, you need to change the conversation.
Stop trying to “convince” your doctor and start partnering with them. You are not a passive patient; you are an active investigator bringing them new data.
Here is a simple, non-confrontational script to use. Do not get emotional. Be calm, firm, and clear.
Start by acknowledging their perspective: “Doctor, I understand why my symptoms look like anxiety or just menopause. I am definitely feeling anxious and not sleeping well.”
Then, pivot by introducing your new data: “However, I’ve been paying very close attention. I’ve realized my heart palpitations are not random. They happen most often at night and seem to wake me up. I often wake up with a gasp or a choking feeling, and then my heart is pounding. This feels like a physical event, not an emotional one.”
Finally, make your specific, non-negotiable request: “I’ve read that sleep apnea in postmenopausal women often presents exactly like this—with insomnia and anxiety instead of loud snoring. Before we treat me for an anxiety disorder, I need to rule out a physical cause. I would like a referral for an at-home sleep study.”
This script does three things:
- It shows you respect their opinion.
- It provides new, specific evidence (palpitations causing the wake-up).
- It names the exact test you need.
This is how you move from being dismissed as “just anxious” to being diagnosed.
Conclusion
Those nighttime heart palpitations aren’t just “in your head,” and they aren’t something you just have to “live with” as part of aging. They are a direct warning sign from your heart.
The most dangerous bedroom habit you can have is passivity—attributing these symptoms to menopause or anxiety while a treatable condition, sleep apnea, silently strains your cardiovascular system.
Your heart health is not negotiable. Listen to the warning. Look at the atypical symptoms, advocate for yourself with your doctor, and demand a sleep study.
Breaking this “habit” of ignoring the signs is the single most important step you can take today to ensure a safer, calmer, and healthier tomorrow.
Share this with a woman in your life who needs to hear this. It could be the wake-up call she needs. Stop letting this bedroom habit control your heart palpitations.

